LIVE UPDATES: Coronavirus - These are the 12 countries and territories on the quarantine-free 'green list'
and live on Freeview channel 276
Scroll down for more on this story.
LIVE UPDATES: Coronavirus NI - One additional death and 65 new infections detected in last 24 hours
Key Events
- One additional death and 65 new infections detected in last 24 hours
- DoH issues advice to anyone under 40 who had AstraZeneca as first dose
- Under-40s are to be offered an alternative to the Oxford/AstraZeneca coronavirus vaccine
- Health chiefs are refusing to confirm or deny if seven people with Indian variant had been vaccinated
These are the 12 countries and territories on the UK government’s ‘green list'


- Portugal (inc. Azores and Madeira)
- Australia
- New Zealand
- Singapore
- Brunei
- Iceland
- Faroe Islands
- Gibraltar
- Falkland Islands
- South Georgia and the South Sandwich Islands
- Saint Helena, Ascension & Tristan da Cunha
- Israel
This is why the PHA is refusing tell you if the seven people infected with the Indian Covid-19 variant had been vaccinated or not
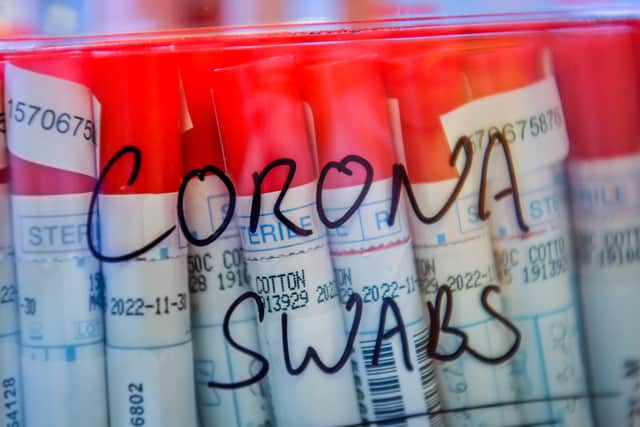

The Public Health Agency (PHA) has explained why it refuses to confirm or deny whether any or all of the seven confirmed cases of the Indian Covid-19 variant in Northern Ireland had been vaccinated before they were infected.
On behalf of our readers throughout Northern Ireland, we put the following specific questions to the PHA earlier today.
- How many of the seven confirmed cases of the Indian variant in Northern Ireland had been fully vaccinated?
- How many of the seven confirmed cases of the Indian variant in Northern Ireland had received at least one dose of a Covid-19 vaccine?
- If applicable, how many of the seven confirmed cases of the Indian variant in Northern Ireland had received the Pfizer or AstraZeneca vaccine?
- How many of the seven confirmed cases of the Indian variant in Northern Ireland had not yet received their first dose of a Covid-19 vaccine?
The PHA responded stating the reason they were refusing to put the information into the public domain is because it could lead to “identification and stigmatisation” of the seven people with confirmed cases of the Indian variant.
“The agency will not be giving specific information on the small number of cases currently identified as it risks identification and stigmatisation and there is no wider public health need,” a PHA spokesperson said.
The spokesperson continued: “If the agency assesses as things progress that it is necessary to take further actions, this will be fully communicated.
“The best way to protect yourself against COVID-19 is to follow all of the public health guidance – practise good hand and respiratory hygiene regularly, keep a distance of two metres from others where you can, wear a face covering where appropriate, and if you are eligible for vaccination please get it.
“It’s also important to remember that if you have symptoms of COVID-19 – a new continuous cough, or a high temperature, or a change in your sense of taste or smell – book a test immediately, and when waiting for your test and test result, ensure that you and household follows the isolation guidance.”
One additional death and 65 new infections detected in last 24 hours


There has been one further death of a patient who had previously tested positive for Covid-19 in Northern Ireland.
The Department of Health said there had also been an additional 65 cases of the virus confirmed in the last 24-hour reporting period.
On Friday morning, there were 62 Covid-19 positive inpatients in hospital, of whom six were in intensive care.
DoH issues advice to anyone under 40 who had AstraZeneca as first dose
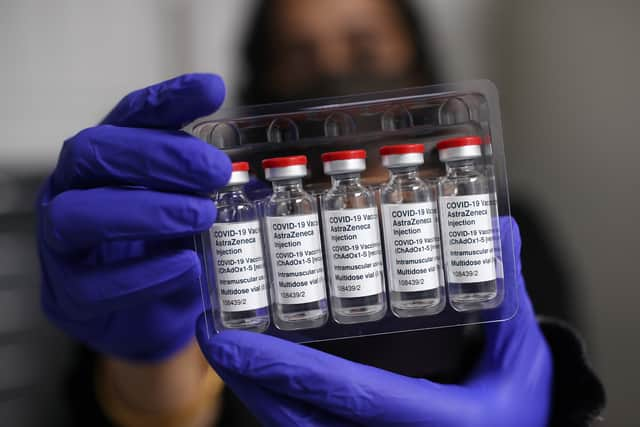

Keep coming forward for your first and second COVID-19 vaccine doses.
That’s the clear advice to the public, as the unprecedented drive to protect the population continues.
Vaccines continue to save lives in Northern Ireland and to protect people from serious illness. The Astra Zeneca vaccine continues to be essential in the successful roll-out of our vaccination programme. Thanks to this programme, close to a million people here have already received their first vaccine dose, helping society to emerge carefully from lockdown.
Following the latest advice from the JCVI (Joint Committee on Vaccination and Immunisation), people aged under 40 will be offered the Pfizer-BioNTech in NI through the regional Trust vaccination centres.
Anyone of any age who has had a first dose of Astra Zeneca should proceed with their second dose of this same vaccine.
The JCVI has advised that those aged under 40 may still make an informed choice to receive the Astra Zeneca vaccine, for instance where no alternative vaccine is available, or where someone has an appointment booked for vaccination in the coming days and may prefer not to reschedule to receive an alternative vaccine.
The JCVI’s updated advice relates to reports of extremely rare adverse events of concurrent thrombosis (blood clots) and thrombocytopenia (low platelet count) following vaccination with the first dose of AstraZeneca vaccine.
The JCVI has updated its risk/benefit advice in relation to age groups, in light of the current low incidence of disease and current and projected availability of alternative vaccines. In light of these factors, Pfizer is now its recommended vaccine for under 40’s.
The change means some logistical alterations to Northern Ireland’s vaccination programme. From Monday, May 10.
* People aged 40 plus can book Astra Zeneca first dose appointments at the SSE Arena vaccination centre and community pharmacies.
* People aged 30-39 can book their Pfizer first dose appointments at the other regional Trust vaccination centres across NI.
* People aged 30-39 can choose to make an informed decision to receive the AstraZeneca vaccine from participating community pharmacies if that is what they prefer or if they decide they would rather not wait to receive an alternative to the AstraZeneca vaccine.
* Anyone aged under 40 already booked for their first vaccine at one of the Trust centres, including the SSE Arena, will have this appointment honoured – with the Pfizer vaccine.
* Anyone of any age who has received an Astra Zeneca first dose should proceed with their second dose of Astra Zeneca. That’s unless they had an extreme adverse reaction to the first dose.
Head of the NI vaccination programme Patricia Donnelly said: “Protecting our adult population through vaccination is a huge and unprecedented undertaking. Logistical challenges are inevitable, but the programme has already proved itself to be highly resilient.
“I would again appeal for patience from the public, as we reset the programme in light of the updated JCVI advice.
“Pfizer supplies remain steady but limited, so our progress with the 30-39 age group will be limited for the next few weeks. Likewise, those under 30 will have to wait a few weeks before being offered appointments for their first dose.”
Chief Medical Officer Dr Michael McBride said: “It is important to reiterate that the potential risk associated with the AZ first dose is extremely rare and that the threat from COVID-19 is much higher for the majority of adults.
“Getting vaccinated against this virus gives us hope – it protects us and helps us to start reclaim normality. I am looking forward to getting my second dose of Astra Zeneca in the near future and I would again encourage everyone to come forward without delay for their first and second jabs when it’s their turn.”
Under-40s are to be offered an alternative to the Oxford/AstraZeneca coronavirus vaccine


Under-40s are to be offered an alternative to the Oxford/AstraZeneca coronavirus vaccine.
The Joint Committee on Vaccination and Immunisation (JCVI) said there is an “extremely small risk” of people suffering blood clots after having the jab, but the risk of serious illness with Covid-19 also drops for younger people as infection rates fall across the country.
While the balance of benefit and risk for the AstraZeneca vaccine is very favourable for older people, it is more finely balanced for younger groups, who do not tend to suffer serious coronavirus illness.
Experts have also assessed the risks from any third wave of Covid in the UK and concluded that that wave is likely to be smaller than previously anticipated.
It came as an expert source said they anticipate approval of the Johnson & Johnson vaccine in the UK shortly.
The Medicines and Healthcare products Regulatory Agency (MHRA) is currently appraising the jab and the review is said to be at an advanced stage.
Regarding AstraZeneca, the JCVI has advised that another vaccine should be offered to under-40s without underlying health conditions where an alternative is available, and as long as it does not cause any substantial delays to the vaccination programme.
Urging people to accept vaccines, it has warned that reductions in uptake or speed of jab deployment will increase the size of any third wave of infection in the UK.
For this reason, it believes any vaccine would be better than no vaccine, even for those under the age of 40.
However, there are thought to be no supply issues with offering the vast majority of younger people alternatives to AstraZeneca.
Professor Wei Shen Lim, Covid-19 chairman for JCVI, said: “Safety remains our number one priority.
“We have continued to assess the benefit/risk balance of Covid-19 vaccines in light of UK infection rates and the latest information from the MHRA on the extremely rare event of blood clots and low platelet counts following vaccination.
“As Covid-19 rates continue to come under control, we are advising that adults aged 18 to 39 years with no underlying health conditions are offered an alternative to the Oxford/AstraZeneca vaccine, if available and if it does not cause delays in having the vaccine.
“The advice is specific to circumstances in the UK at this time and maximises use of the wide portfolio of vaccines available.
“The Covid-19 vaccines have already saved thousands of lives and the benefit for the majority of the population is clear – if you are offered the vaccine, you should take it.”
Up to April 28, the MHRA had received 242 reports of blood clots accompanied by low blood platelet count in the UK, all in people who had the AstraZeneca vaccine, out of around 28.5 million doses given.
These clots occurred in 141 women and 100 men aged from 18 to 93, with 49 deaths. Six cases have been reported after a second dose.
A particular type of brain blood clot – cerebral venous sinus thrombosis (CVST) – was reported in 93 cases (with an average age of 47), and 149 had other major thromboembolic events (average age 55) accompanied by low blood platelet count.
The overall incidence of blood clots with low platelets after a first dose is put at 10.5 per million doses, and about one in a million for a second dose.
For those aged 40 to 49 the incidence is 10.1 per million doses, and 17.4 per million for those aged 30 to 39.
Overall, the death rate per million doses is 2.1, but is 4.5 for those aged 30 to 39.
MHRA chief executive Dr June Raine said: “Public safety is always at the forefront of our minds and we take every report seriously.
“Our position remains that the benefits of the Covid-19 vaccine AstraZeneca against Covid-19, with its associated risk of hospitalisation and death, continues to outweigh the risks for the vast majority of people.
“The balance of benefits and risks is very favourable for older people but is more finely balanced for younger people and we advise that this evolving evidence should be taken into account when considering the use of the vaccine, as JVCI has done.”
According to Public Health England (PHE), the vaccine programme is estimated to have prevented more than 10,000 deaths in England alone by the end of March.
Health experts are urging everyone who has had a first dose of AstraZeneca and not suffered a clot to have a second dose of the same jab, irrespective of their age.
The MHRA said that, as a precautionary measure, anyone who has a severe headache which is not relieved with painkillers or is getting worse, should seek prompt medical attention at any point from around four days to four weeks after vaccination.
The same goes for a headache that feels worse when a person lies down or bends over, a headache that is unusual and occurs with blurred vision, feeling or being sick, problems speaking, weakness, drowsiness or seizures, a rash that looks like small bruises or bleeding under the skin, and shortness of breath, chest pain, leg swelling or persistent abdominal pain.
Health chiefs are refusing to confirm or deny if seven people with Indian variant had been vaccinated
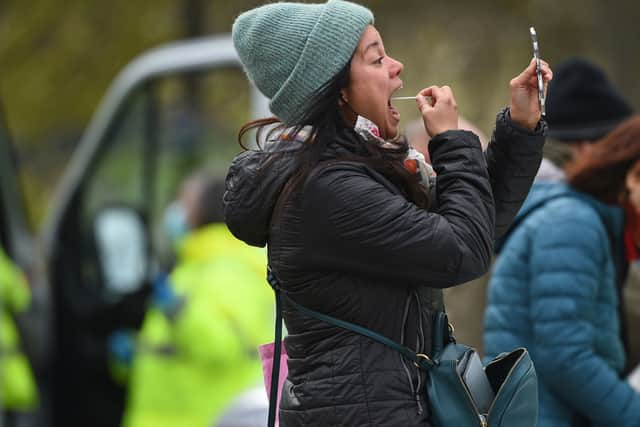

The Public Health Agency (PHA) in Northern Ireland is refusing to tell the public if any of the seven people who have tested positive for B.1.617, also referred to as the Indian variant, had been vaccinated before they were infected.
The seven cases of B.1.617 in Northern Ireland were confirmed on Thursday by the Department of Health (DoH).
Some media organisations have asked if any of the seven confirmed cases had been vaccinated before they became infected with the variant.
Speaking on Thursday, Chief Medical Officer for Northern Ireland, Dr. Michael McBride said: “This news is not entirely unexpected and plans are in place for such an eventuality.
“While preventative measures – including travel restrictions – are very important, the assessment is that these will delay rather than permanently prevent the spread of variants already detected elsewhere on these islands.
“Confirmation of these cases does not mean this variant is going to become the most prevalent or the dominant strain in Northern Ireland.
“It does, however, highlight why caution is still essential in relation to COVID-19.
“The most effective way to stop variants developing or spreading is to keep pushing down infection rates and transmission of the virus in our community.
“All variants spread in the same way. We protect ourselves and others by following public health advice and getting vaccinated when our turn comes.
“Social distancing and limiting the number of contacts we have are still vitally important. So too are wearing a face covering and washing hands well and often. Also, please always remember the particular risks from indoor settings, especially those that are crowded and have poor ventilation.”
We have contacted the PHA for a response.
Comment Guidelines
National World encourages reader discussion on our stories. User feedback, insights and back-and-forth exchanges add a rich layer of context to reporting. Please review our Community Guidelines before commenting.
